Treatments
Escape joint pain with stem cell therapy. Rediscover mobility, live pain-free.
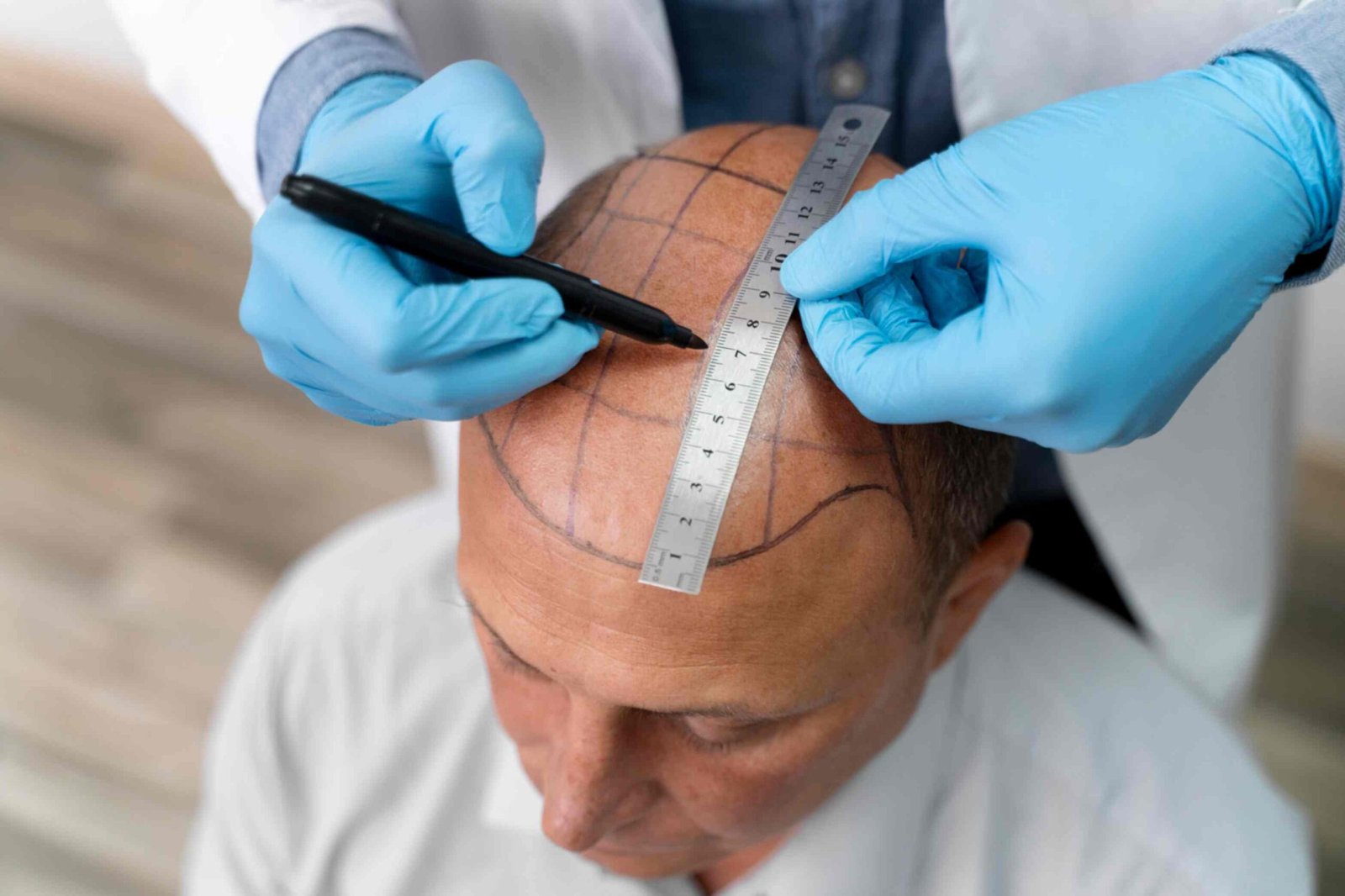
Reclaim your confidence with stem cell therapy for alopecia. Revive your self-esteem.
Osteoarthritis – Joint pain
Osteoarthritis is a common degenerative joint disease characterized by the gradual breakdown of cartilage, the flexible and protective tissue that covers the ends of bones within a joint. Cartilage serves as a cushion and allows smooth, frictionless joint movement.
In osteoarthritis, the cartilage begins to deteriorate and wear away over time. As a result, the bones can rub directly against each other, causing pain, swelling, stiffness, and a reduced range of motion in the affected joint. Osteoarthritis most commonly affects weight-bearing joints, such as the knees, hips, and spine, but it can also impact other joints like the hands, fingers, and toes.
The exact cause of osteoarthritis is multifactorial and can include factors such as age, genetics, joint injury, obesity, and joint overuse. It is a progressive condition that can worsen over time, leading to significant discomfort and functional limitations.
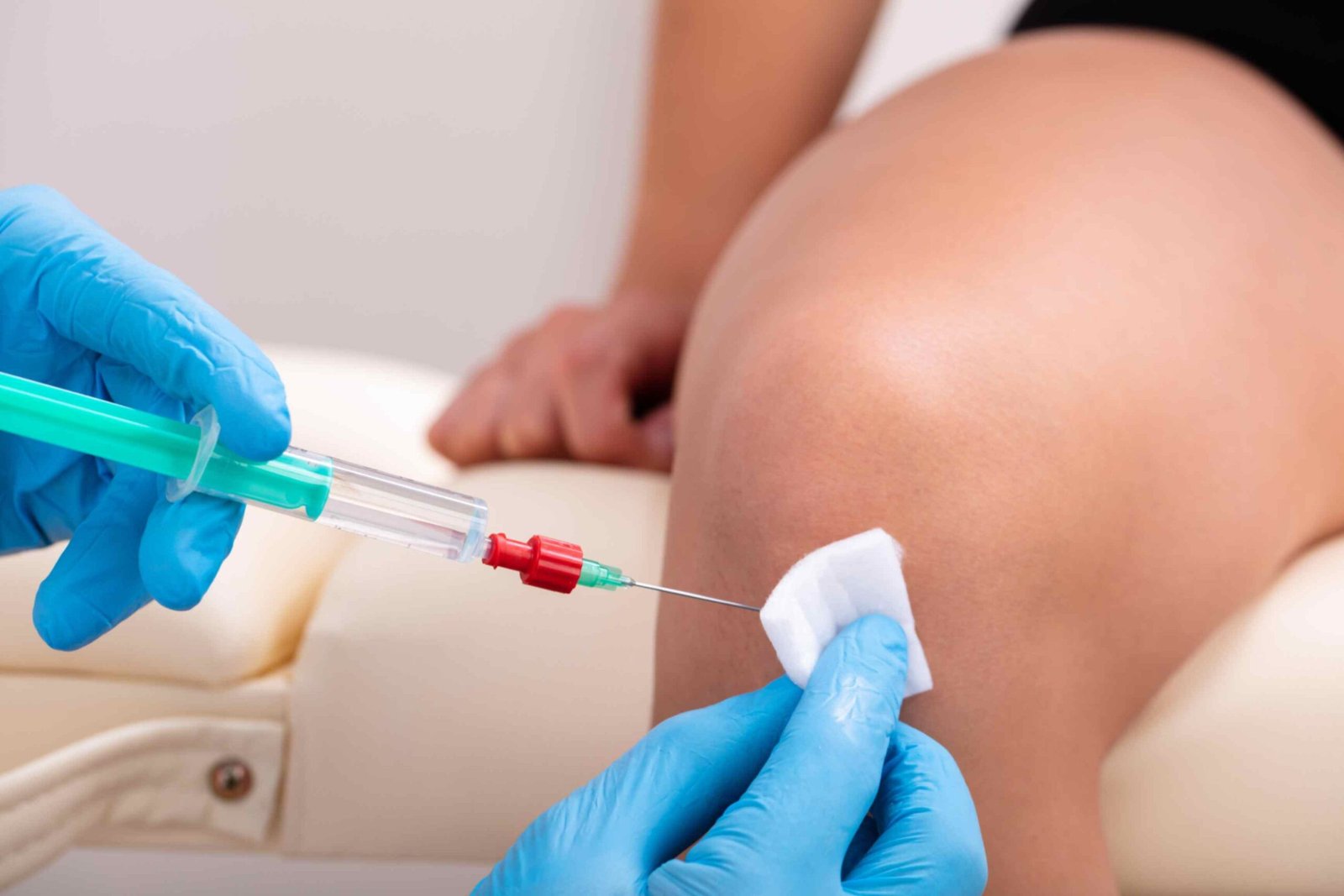
Technically, how is it done?
Injecting stem cells is a medical procedure where stem cells, typically derived from a patient’s own body or from a donor, are introduced into a specific area, such as a joint or tissue, through a needle or catheter. This procedure is used in regenerative medicine to promote tissue repair, reduce inflammation, and potentially treat various medical conditions.
Bibliography
1. Intra-Articular Injection of Autologous Adipose Tissue-Derived Mesenchymal Stem Cells for the Treatment of Knee Osteoarthritis. March 5, 2019. Woo-Suk Lee, Hwan Jin Kim, Kang-Il Kim, Gi Beom Kim, Wook Jin.
2. Mesenchymal Stem Cell-Derived Exosomes and Intervertebral Disc Regeneration. June 30, 2022. Basanta Bhujel, Hae-Eun Shin, Dong-Jun Choi, Inho Han.
Timeline
1. Patient Evaluation:
Before the procedure, the patient undergoes an evaluation, which may include a review of medical history, a physical examination, and possibly imaging studies (e.g., X-rays, ultrasound) to assess the joint’s condition and identify the source of pain or inflammation.
2. Informed Consent:
The healthcare provider explains the procedure, its potential risks and benefits, and obtains the patient’s informed consent.
3. Preparation:
The patient is positioned comfortably, and the skin over the targeted joint is cleaned and sterilized to reduce the risk of infection.
4. Local Anesthesia:
In many cases, a local anesthetic is administered to numb the skin and surrounding tissues, which helps minimize discomfort during the injection.
5. Needle Insertion:
A thin sterile needle is inserted directly into the affected joint under guidance from imaging techniques such as fluoroscopy, X-rays, or ultrasound. The choice of imaging depends on the joint’s location and the healthcare provider’s preference.
6. Medication Injection:
The healthcare provider injects the STEM CELLS into the joint space.
7. Post-Injection Observation:
After the injection, the patient may be monitored for a short period to ensure there are no immediate adverse reactions.
8. Recovery and Aftercare:
The patient is typically allowed to resume normal activities, but they may be advised to take it easy for a day or two to rest the treated joint. Pain management is recommended to manage any post-injection discomfort. Patients may also receive instructions for post-injection care and follow-up appointments.
Unlock now your regeneration!
-
Unlock now your regeneration!
-
Unlock now your regeneration!
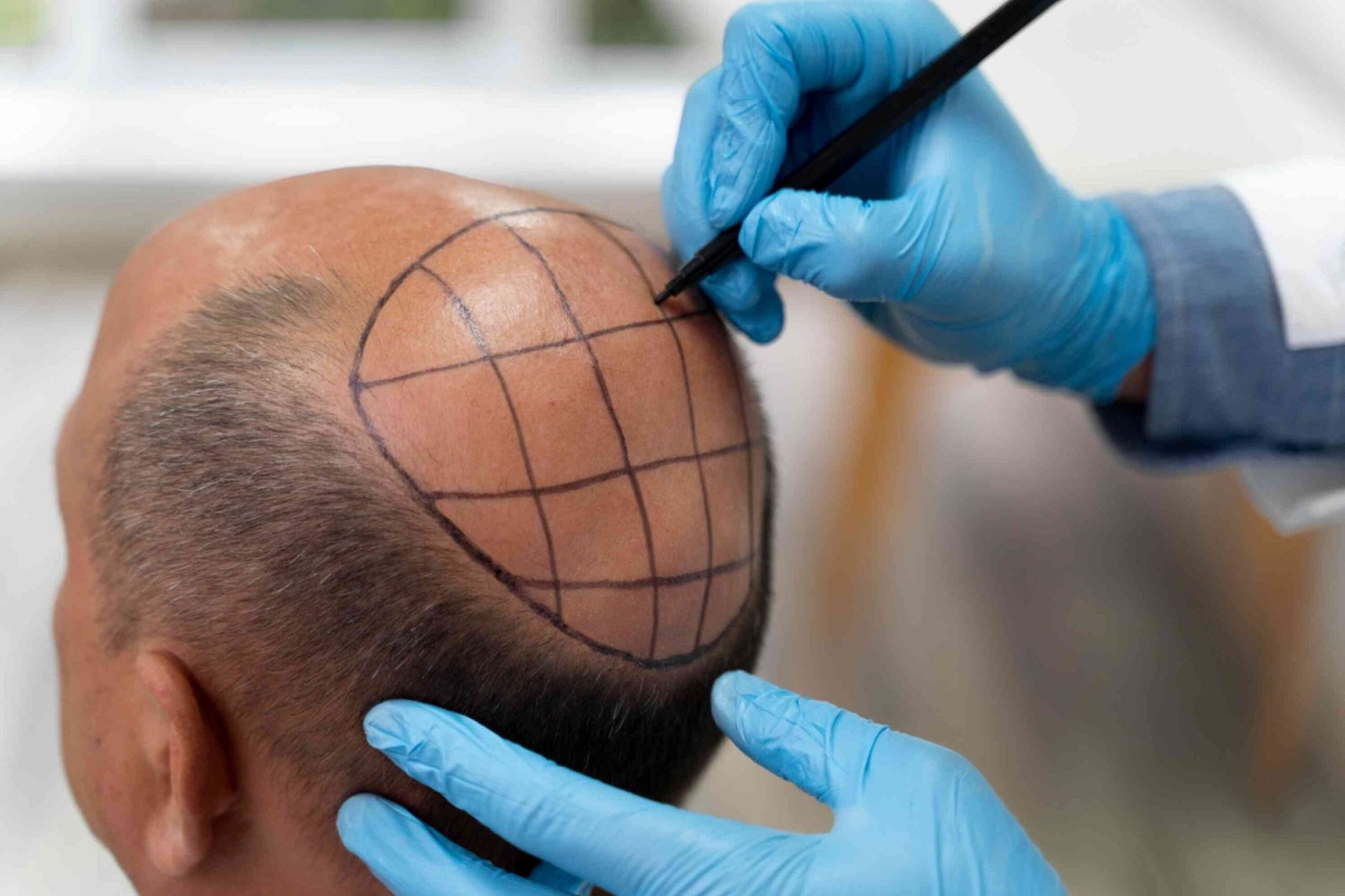
Alopecia
“Stem cell therapy for alopecia” involves using stem cells, like mesenchymal stem cells or platelet-rich plasma, to stimulate hair follicles and promote hair growth.
“Hair transplantation” is a surgical procedure where hair follicles from one part of the body are moved to areas with hair loss.
Combining stem cell therapy and hair transplantation involves using stem cell treatments to enhance the success of hair transplantation. Stem cells may be used to prepare the recipient area and promote a healthier environment for transplanted hair follicles.
This combination approach is being explored to potentially improve the outcomes of hair restoration procedures, although its effectiveness is still being studied. It’s essential to consult with a qualified medical professional for personalized advice on treating alopecia.
Technically, how is it done?
Certainly, here’s a concise explanation of the combination of stem cell therapy and hair transplantation for alopecia treatment:
Consultation: Meet with a specialist to assess your hair loss and determine the best treatment plan.
Stem Cell Therapy: Stem cells, such as PRP or ADSCs, are prepared and injected into the scalp to promote hair growth. Hair Transplant If needed, a hair transplant procedure is performed, where hair follicles are taken from one area and transplanted into the balding areas.
Recovery and Follow-up: Follow post-operative care instructions, and continue to see your specialist for check-ups and guidance on hair care. This combination approach aims to enhance the success of hair restoration, but results can vary, so consult a qualified professional for personalized advice.

Bibliography
1. Advances in Regenerative Stem Cell Therapy in Androgenic Alopecia and Hair Loss, 16 May 2019. Pietro Gentile, and Simone Garcovich.
2. Regenerative medicine strategies for hair growth and regeneration. 15 October 2022. Yusuke Shimizu, Edward Hosea Ntege, Hiroshi Sunami, Yoshikazu Inoue.
3. Advancing Regenerative Cellular Therapies in Non-Scarring Alopecia. 10 March 2022. Talagavadi Channaiah Anudeep, Madhan Jeyaraman 2 4 5, Sathish Muthu, Ramya Lakshmi Rajendran, Prakash Gangadaran, Prabhu Chandra Mishra, Shilpa Sharma, Saurabh Kumar Jha, Byeong-Cheol Ahn.
Timeline
The Priapus Shot, commonly known as the P-Shot, is a medical procedure designed to improve sexual performance and treat erectile dysfunction (ED) using MSC therapy. Here’s an overview of how a P-Shot is administered:
1. Patient Evaluation:
The patient undergoes a thorough evaluation, including a medical history assessment and a physical examination. This helps determine if the P-Shot is an appropriate treatment for the specific case of ED or sexual performance concerns.
2. MSC Preparation:
The MSC is prepared by spinning the blood sample in a centrifuge to separate the plasma, which is rich in platelets and growth factors. This concentrated MSC is what will be used in the P-Shot.
3. Local Anesthesia:
A topical numbing cream or local anesthetic is applied to the penis to ensure the procedure is as comfortable as possible for the patient.
4. MSC Injection:
Using a fine needle, the healthcare provider injects the concentrated MSC directly into various locations in the penis, typically in the corpus cavernosum, which is the area responsible for erections. The MSC contains growth factors that can stimulate tissue regeneration and blood vessel formation.
5. Post-Injection Observation:
After the injection, the patient is typically monitored for a brief period to ensure there are no immediate adverse reactions. Most patients can resume normal activities shortly after the procedure.
6. Recovery and Aftercare:
Over time, the MSCs promote tissue repair, increase blood flow, and improve penile function. Patients may start to see improvements in their sexual performance within a few weeks to months after the procedure.
Unlock now your regeneration!
-
Unlock now your regeneration!
-
Unlock now your regeneration!